
Credentialing software for healthcare organizations to manage provider credentials, expirations, verifications, and compliance documentation.
Vendor
MedTrainer
Company Website
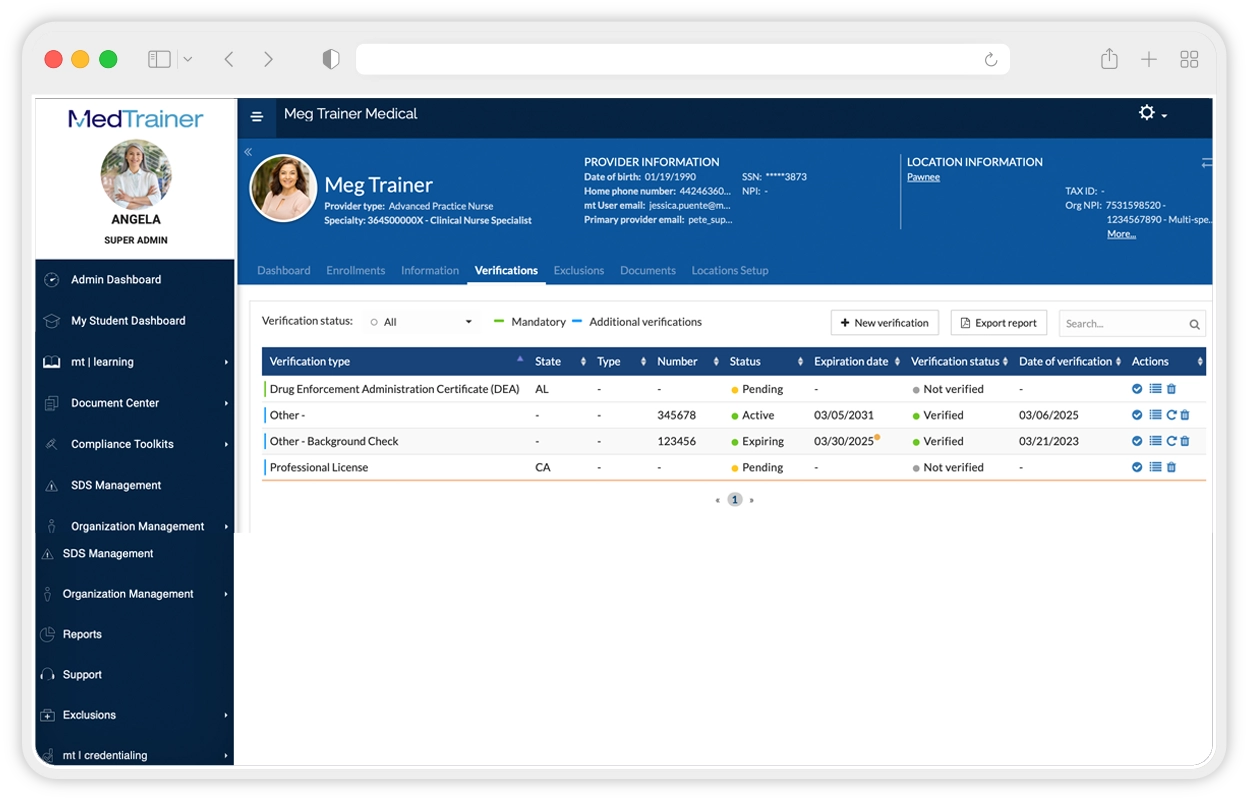
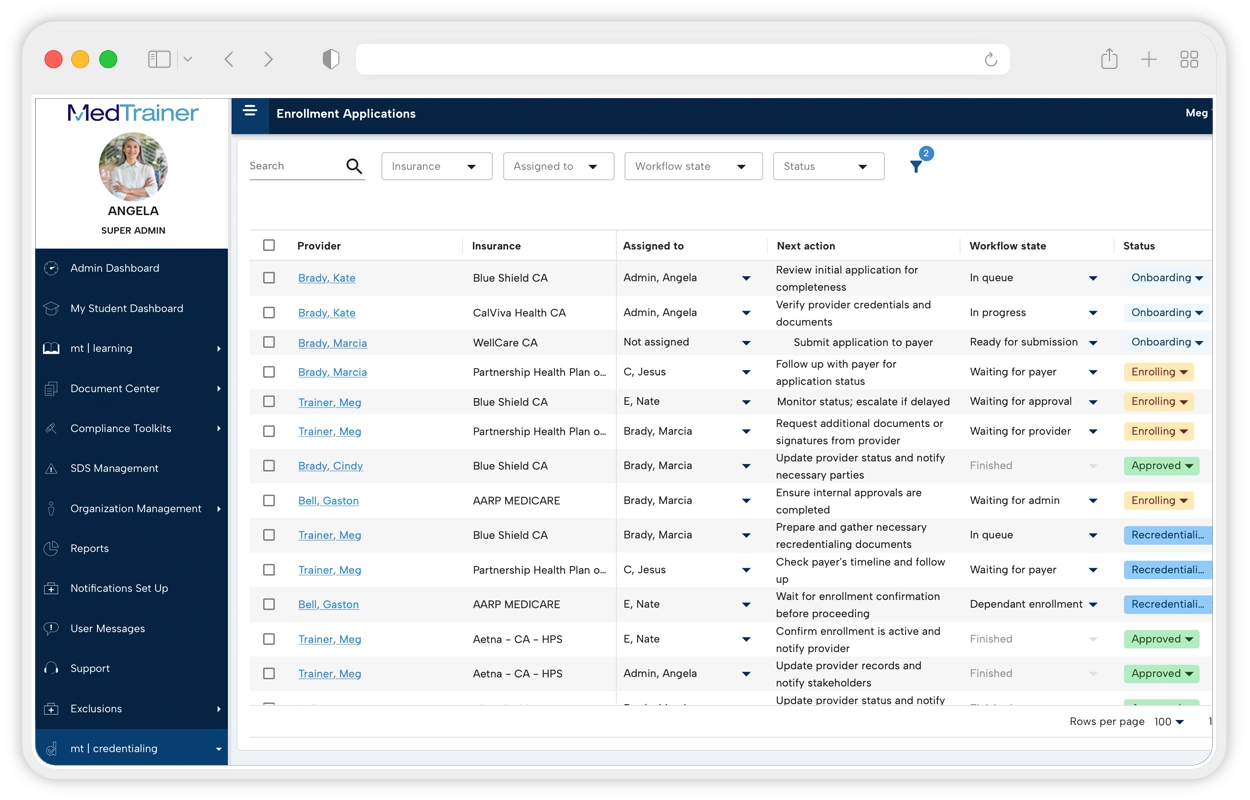
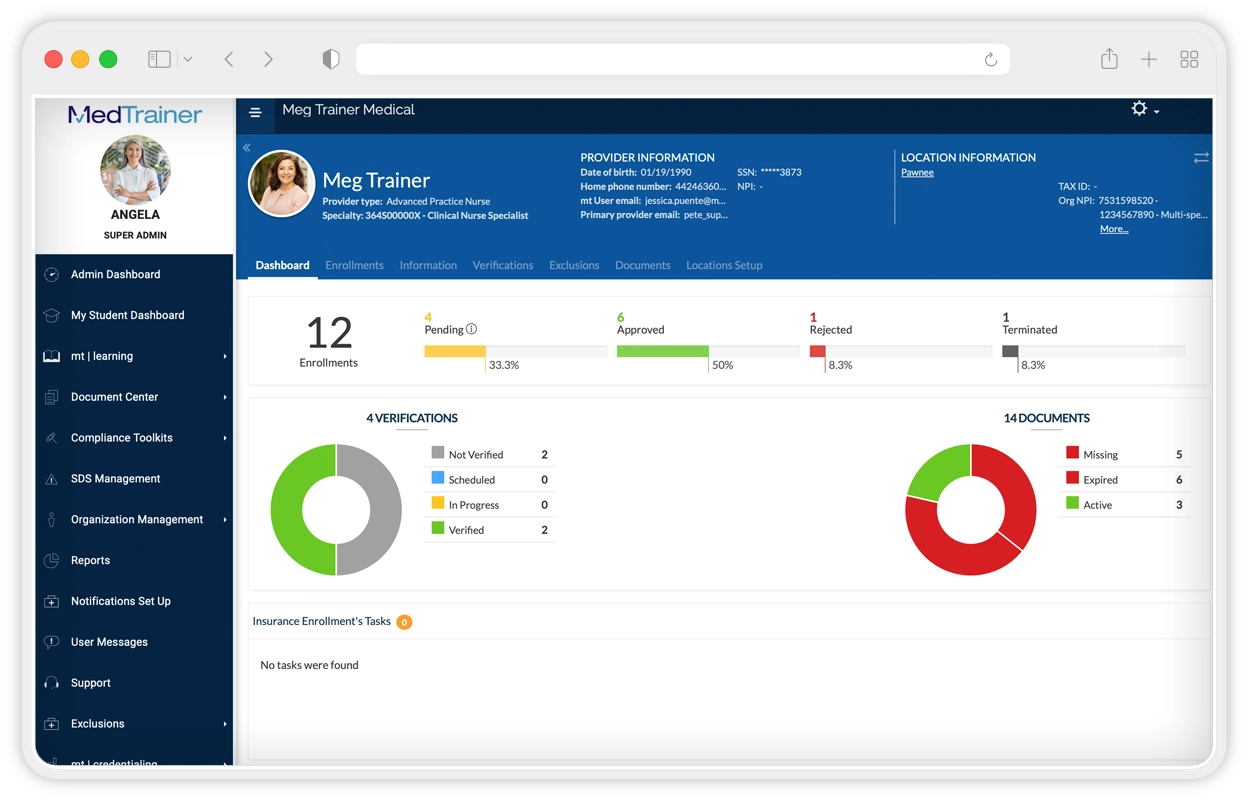
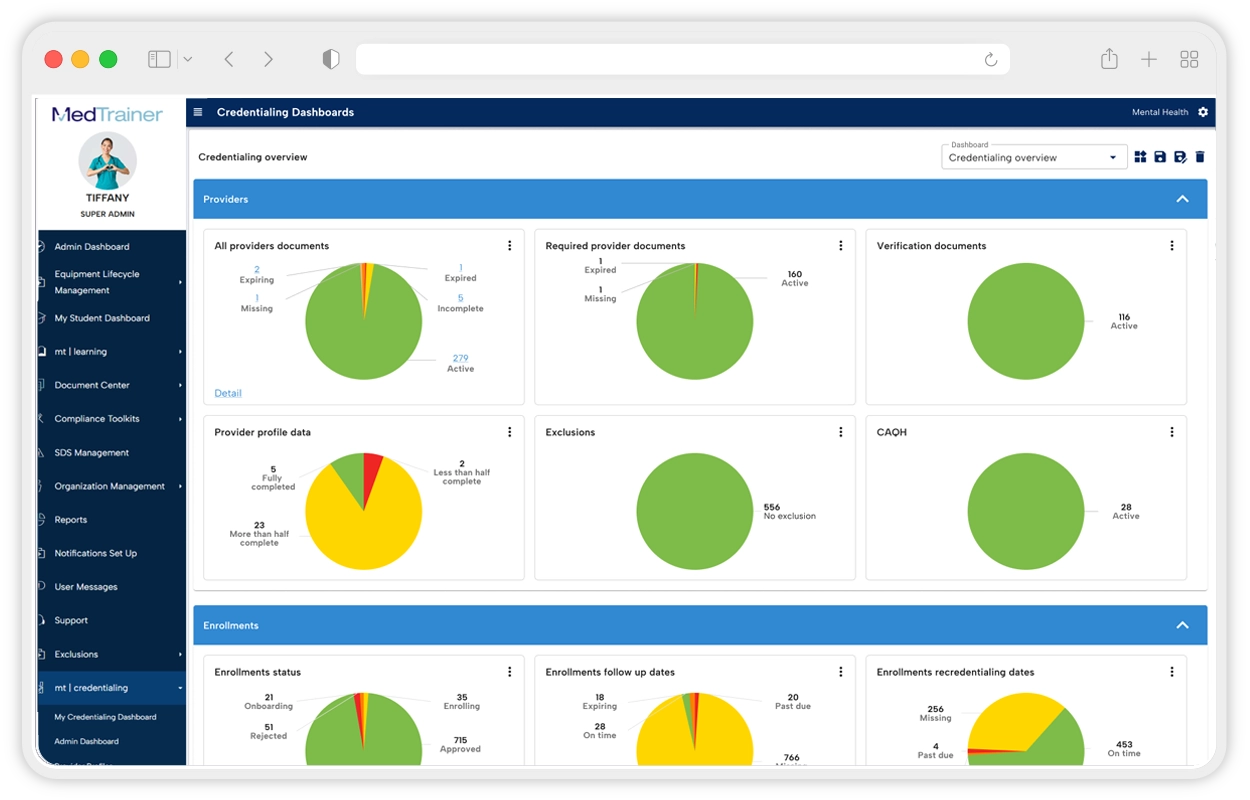
MedTrainer Credentialing is a software platform designed to manage and maintain credentialing information for healthcare providers. It provides a centralized system to store, track, and verify practitioner credentials required for clinical practice and regulatory compliance. The platform structures credentialing workflows by organizing licenses, certifications, education, work history, and other required documentation. It enables healthcare organizations to monitor credential status, manage renewals, and maintain up‑to‑date provider records across facilities and roles. MedTrainer Credentialing is intended to reduce manual credential tracking, improve data accuracy, and provide a clear system of record for credentialing activities. It supports ongoing compliance by tracking expirations and maintaining documentation needed for audits and inspections.
Key Features
Provider Credential Records
Centralizes practitioner data.
- Storage of licenses and certifications
- Structured provider profiles
Expiration Tracking
Monitors credential validity.
- Automated expiration tracking
- Alerts for upcoming renewals
Primary Source Verification Support
Supports verification processes.
- Documentation of verification steps
- Tracking of verification status
Workflow Management
Structures credentialing tasks.
- Credentialing task assignments
- Status tracking across stages
Document Management
Organizes supporting materials.
- Secure document storage
- Version and history tracking
Reporting and Oversight
Provides credentialing visibility.
- Credential status reports
- Compliance and readiness views
Benefits
Improves Credential Accuracy
Reduces errors and gaps.
- Centralized data management
- Standardized credential records
Supports Regulatory Compliance
Aligns with healthcare requirements.
- Documented credential history
- Readiness for audits and reviews
Reduces Administrative Work
Simplifies credentialing tasks.
- Automated expiration reminders
- Structured workflows
Increases Visibility
Clarifies credential status.
- Real‑time credential tracking
- Organization‑wide oversight
Supports Provider Lifecycle Management
Tracks credentials over time.
- Initial credentialing
- Ongoing recredentialing